Coast nurses hit ‘compassion fatigue’ with the unvaccinated as COVID’s 4th wave surges
The hum of exhaust systems sucking air out of contaminated rooms filled an ICU at Ocean Springs Hospital on a recent Tuesday.
Health care workers changed in and out of personal protective equipment in a continuous loop, entering rooms only long enough to flip COVID-19 patients from their backs to their bellies; a process called proning that helps them breathe.
The bodies that lay unconscious were not elderly, they appeared middle-aged.
Every air-tight room with a ventilator in front of the door was housing a severely ill patient with the coronavirus. There were seven in the unit, but 57 across Singing River Health System’s three hospitals.
Mississippi health care workers are in the midst of what one Singing River ICU nurse called a bout of PTSD and another called a bad dream: the fourth wave of COVID-19.
But it’s different than previous surges.
This round, compassion is running dry. Ninety-five percent of the hospitalized patients at Singing River hospitals are unvaccinated.
This wave was preventable, according to the data and medical experts. Nurses now find themselves frustrated by persistently low vaccination rates — a discouraging trend that could cause more variant spikes and more death.
Mississippi’s vaccination rate is 34%, according to data updated this week, compared to the 49% national average. The Coast’s rate is even lower.
“I knew that it was going to be another wave, almost — if not worse — than we had last year,” said Jen Sartin, an ICU nurse who recently resigned from critical care.
“And this time is different, because knowing that most of the cases are from unvaccinated patients, it adds a level of frustration that wasn’t there before.”
She left when COVID patients jumped from three to eight in a week.
“It’s just emotionally and mentally exhausting and defeating. I literally cried in the unit, in the ICU. And then I got in my car and I cried the whole way home. And then I got home and I cried some more.”
The strongest reason she had for resigning, Sartin said, was she didn’t want to be a nurse that loses compassion for her patients.
“I can’t take care of patients that I am angry with,” she said. “Even patients with addictions and things like that — that’s a disease too, that’s easier to take care of. For whatever reason, especially political reasons, [people] are choosing not to get vaccinated and still end up in here.”
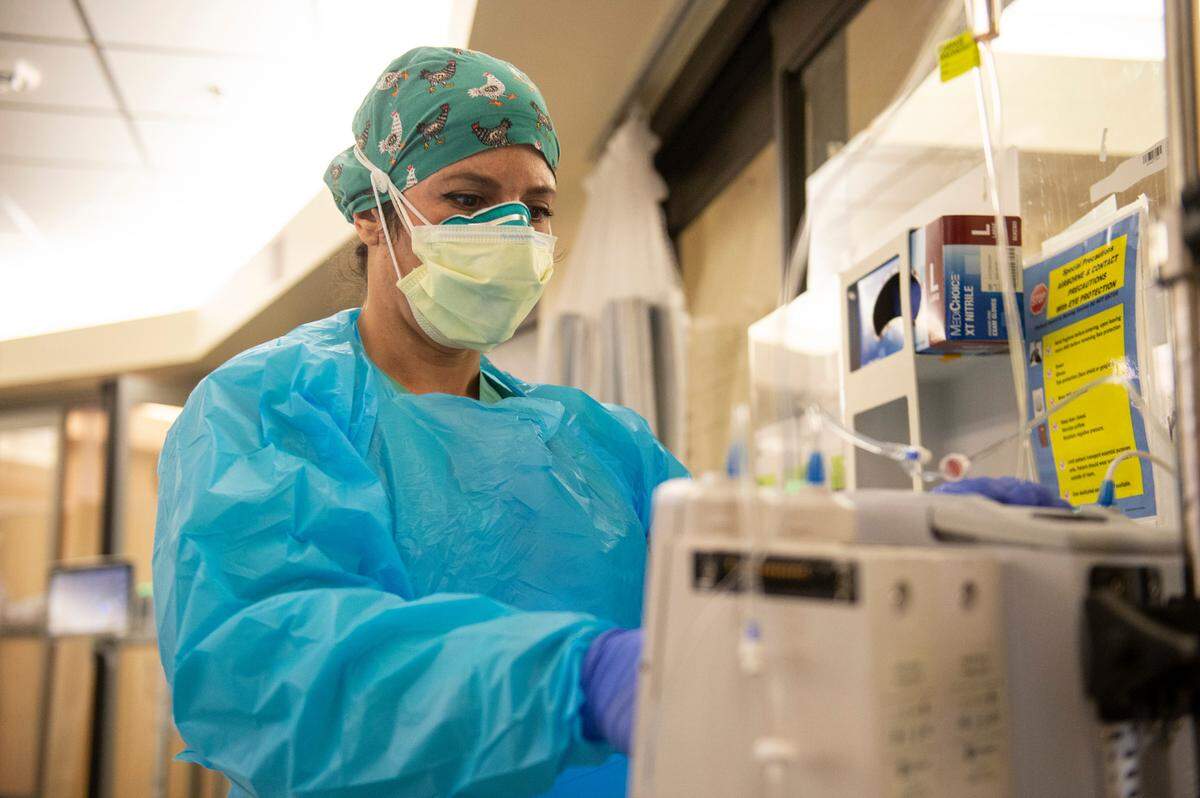
Across Singing River’s hospital locations in Ocean Springs, Pascagoula and Gulfport, ICUs are filling up. Emergency rooms have hours-long wait times. Nursing staffs are short and fatigued.
“This is pretty much how it is in all our surrounding hospitals as well. We’re not the exception,” said Ijlal Babar, pulmonologist and director of Pulmonary Critical Care at Singing River.
Younger patients in ICU
This fourth, delta variant wave of COVID is also distinct because it’s impacting significantly younger age groups. The average age of hospitalized patients at Singing River is currently 49, compared to 67 during the prior waves.
Four children have now died of COVID in Mississippi, State Medical Officer Dr. Thomas Dobbs announced last week.
“This round, we have a 39-year-old female that has fought for about a month now…,” said Singing River ICU nurse Theresa Wolfe. “She’s been scared to death that she’s going to die. She did not get the vaccine.”
When Wolfe left her shift last week, it seemed like things were starting to look up for the patient.
“She’s now on a ventilator with 100% oxygen. Four days later, that’s where she’s at. Is she going to come out of this? We don’t know. We walked in this morning and intubated a patient right off the bat. Emergently. Are these people going to make it? We don’t know.”
The fourth wave certainly hasn’t peaked yet, Babar said. The doctor said it might take two to three months to settle down, once people either develop immunity after they get an infection or if there’s a “miracle,” and more South Mississippians get vaccinated.
Then, if the population still isn’t vaccinated, another variant could take hold.
Fourth wave’s toll on health care workers
Singing River Health Systems CEO Lee Bond teared up as he described the effect of the current COVID surge on his health care staff, especially the nurses.
“While the world is going on about its business, there are places here and throughout Mississippi and this region where a nurse is having to have the unbearable pain of not knowing how badly COVID might affect their patient,” Bond said.
“I would want the public to know that nurses and clinicians are suffering greatly right now, and I think the world has sort of lost sight of that.”

Wolfe, who has been a nurse with Singing River for 21 years, said she’s developed mental and physical health issues from the past year.
“My stress level is higher, my depression is higher, I have actually been on medications… as well as weight. Let’s not forget the weight. Everybody says the ‘COVID 10,’” she said.
“I have been working at getting back to the gym, because that does help your stress relief and helps with bad anxiety and I can see that.”
Sartin is just one of a few nurses who have decided they can’t endure another wave.
“It was a really hard decision for me to decide to leave, because I know people still need to be taken care of, but when it came down to it, I knew that I was not going to be healthy in the process,” she said. “My mental health is starting to really decline. I started getting headaches and sleepless nights, and it was the more COVID patients that would come in, the worse things got.”
‘To see the actual faces of these patients’
Wolfe said that a lot of patients she sees, especially the young ones, haven’t gotten the vaccine because they think they’re “superman,” among other reasons.
But Babar described in detail what COVID looks like for patients sick enough to be in the ICU. It’s very real and very lonely, he said, for all age groups. Patients cannot see their families, and nurses can only stay in their rooms for limited amounts of time.
For many, the only way to get breath circulating is to have nurses come into their rooms to “prone” them every eight to 16 hours. It’s uncomfortable, especially for obese people.
“When you keep someone prone for days on end, they start breaking down. Their faces start breaking down. They get sores,” Babar said.
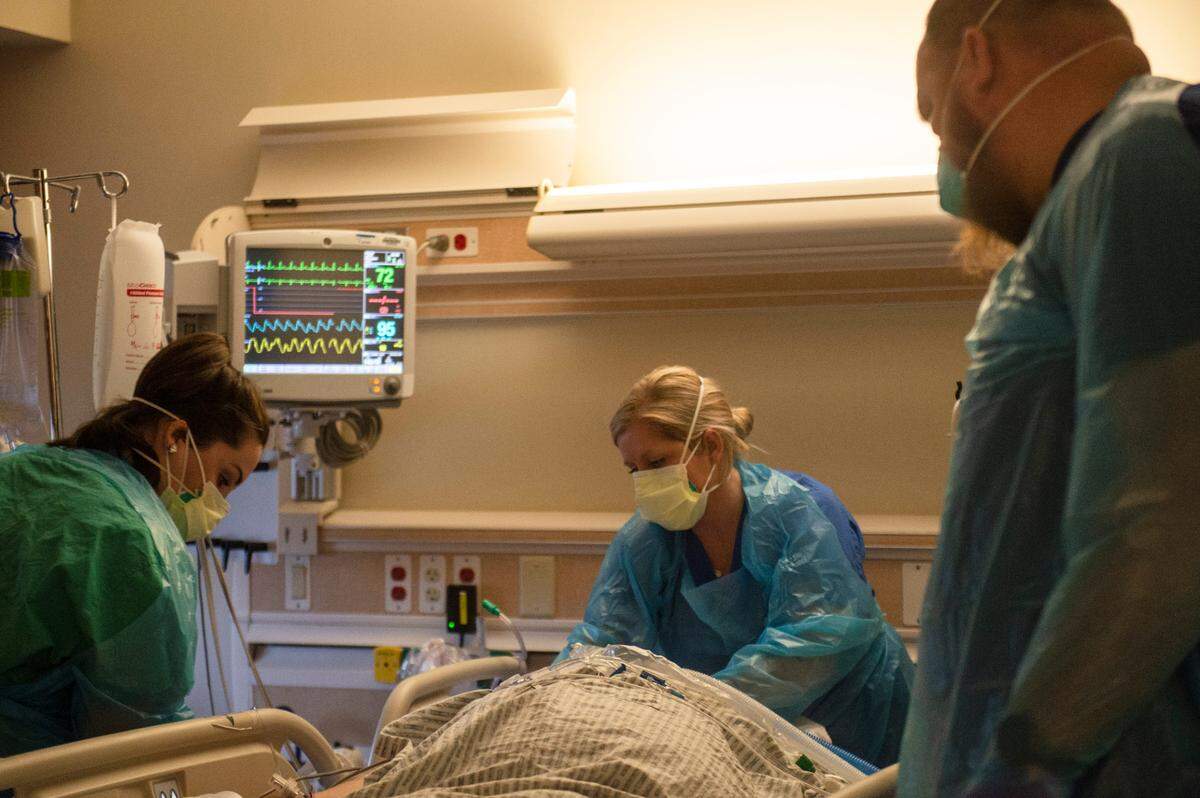
When patients reach a point where they need a ventilator, they usually spend weeks to months hooked up. In many cases, they’re not just sedated but paralyzed. During previous waves of COVID, someone’s chance of survival if put on a ventilator was about 55%.
“As we’re putting these patients on the ventilator, we know in our minds that half of them aren’t going to walk out of here,” he said.
That low survival rate and intense recovery is part of what’s wearing down the health care workers.
“I almost wish that there was a way for the public to see the actual faces of these patients. To see them intubated, to see them bleeding, to see everything that happens that’s associated with it,” Sartin said.
“Because it’s not just being on a ventilator. It’s strokes and clots and all these other issues and it’s terrible.”
Some stay vaccine-hesitant, even after hospitalization
Some patients are remorseful they didn’t get the vaccine, the nurses said, but not all.
“Several nurses have talked to [patients] and their families, you know, ‘please go get the vaccine’ … Some are not, even after they’ve gone through this. And we see the sickest of the sick. So we don’t get to see that many that walk out of here,” Wolfe said.
Babar also runs a pulmonary clinic, where he said a few people come nearly every day who are unvaccinated. Those who haven’t gotten the shot are “adamant” about not getting it, he said.
“One person’s words to me were, she would rather die than get vaccinated.”
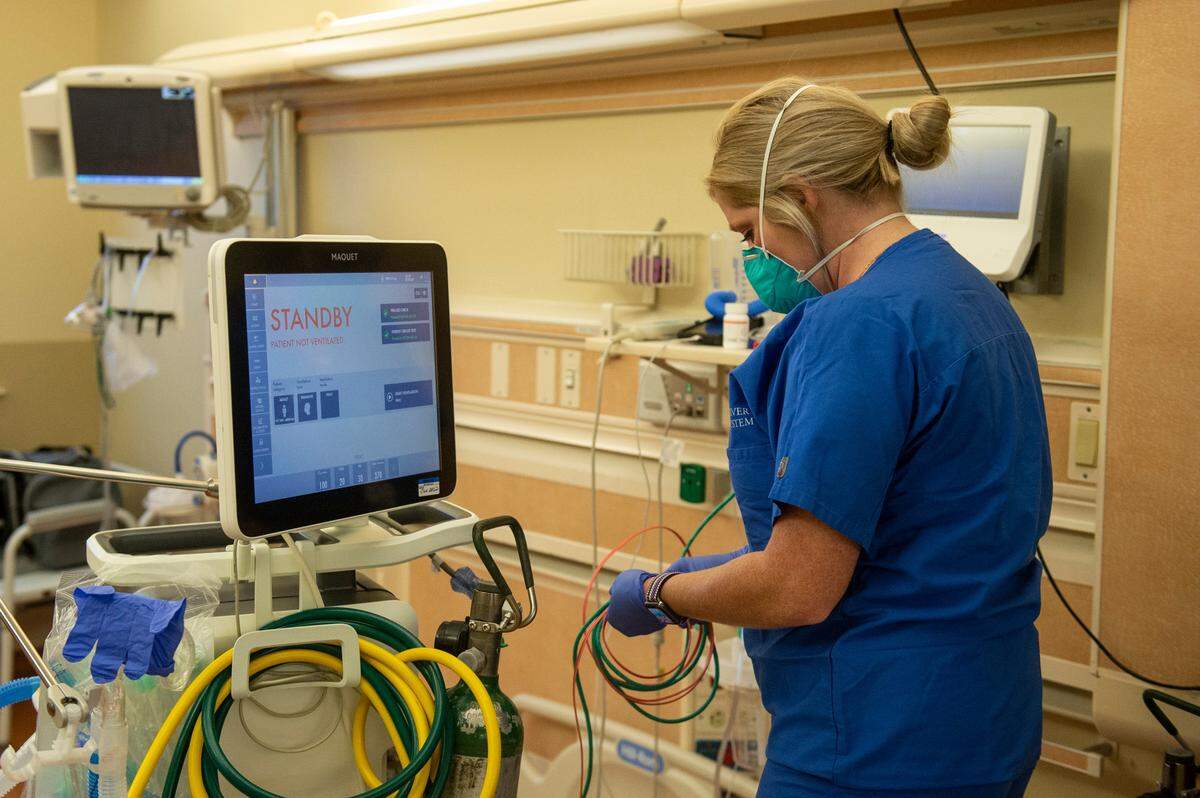
What the health care workers hear most often on vaccine hesitancy: there’s not enough research, that they’ve already had the infection so they don’t need to get a vaccine, that a microchip might be placed inside of them and infertility. The biggest hesitation is that they don’t want to be told by the government that they have to get it.
But the nurses said they’ve also heard a lot of regret from patients who didn’t think the virus was real.
“If they have any kind of regret or change of heart, you’ll hear about that before they get intubated, when they’re still struggling,” Sartin said.
From ‘Chick-Fil-a’ of vaccinations to incentives
For the sake of nurses, Lee Bond has helped lead the vaccine charge in South Mississippi.
“If it were not for the challenges that the nurses on the front line were facing, I would not be advocating it as much as I am,” he said.
When doses first became available to the public, he said Singing River became the “Chick-Fil-a” of vaccinations, offering drive-thru options and other wide-scale events to get shots in the arms of everyone eligible.
But demand dropped off, until a recent uptick in vaccinations.
A Louisiana judge this week offered some probation candidates the option to get a vaccine instead of performing community service. That’s how Bond sees this issue: an act of service.
“Do it for them. Be selfless, We’re in a selfish world. Everybody cares about themselves. And what I am trying to advocate is, think about other people a little bit. Not just a person you might infect, but think about the nurses who are sitting there in the hospital caring for people that don’t have to be in here,” he said.
Bond, who was born in the Pascagoula hospital of the health system he’s now spent three years overseeing, is most frustrated with the politicization of the vaccine issue. As a South Mississippian, he respects personal choice, but he repeatedly said he doesn’t understand the disregard for others being displayed.
“Some people aren’t going to, and I respect their choice. But that choice has an impact on nurses and other caregivers who are right now struggling with life and death every day,” he said.
“You don’t hear me out there saying, get the vaccine, or you’re a bad person. I’m just saying, if you’ve been on the fence about it, think about it,” Bond said. “Please think about it for the sake of the people who are going to have to take care of you.”
Sartin agreed that vaccination is the best way to thank nurses for the work they’ve done over the past year and a half.
“The whole, ‘health care heroes’ thing, that was nice and everything. But that’s never what any of us needed. We needed people to wear their masks… now we need people to get shots. That’s how you show us you appreciate everything that we’ve done,” she said.
This article is supported by the Journalism and Public Information Fund, a fund of the Gulf Coast Community Foundation.
