It’s ‘survival of the fittest’ at a Coast ICU where COVID patients are ‘younger and sicker’
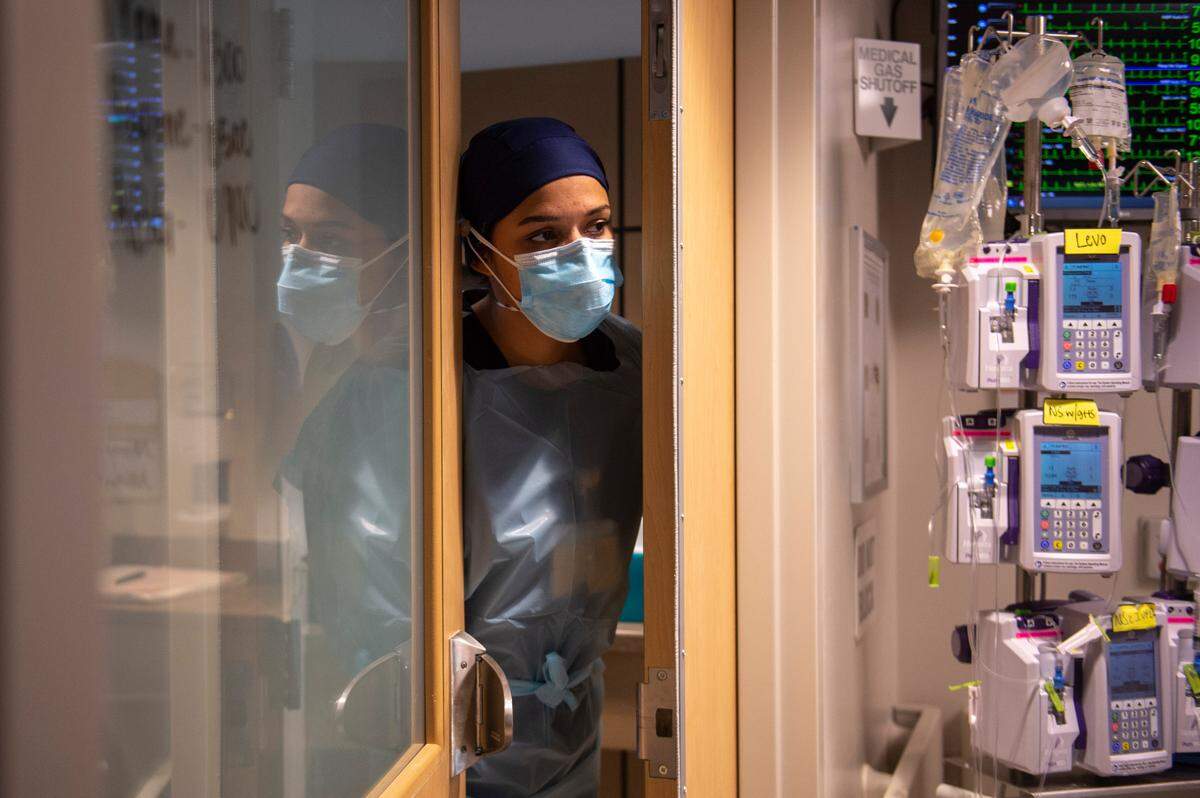
When Mississippi Gov. Tate Reeves posted on social media last Wednesday that the “real challenge” for hospitals during COVID-19’s deadly fourth wave is health care staffing, not physical beds, several nurses in Memorial Hospital at Gulfport’s intensive care unit began to laugh.
“We have five right now waiting to get into the ICU,” said registered nurse Miranda Lewis, pointing to her computer screen with a trailing list of COVID patients in the hospital.
The Sun Herald first spoke with Lewis six months ago, when the hospital was learning how to adapt to the virus by creating more ICU space and commissioning incentives to bring on more staff. Now she was working in one of Memorial’s two ICU units, an expansion that was that wasn’t even open during that time. The hospital has also added overflow intensive care beds.
“We don’t have one bed available.”
Staffing, too, is a booming issue for Memorial and other hospitals along the coast. But Lewis and other Memorial health care professionals said the sheer volume of local patients needing intensive care because of the wildly transmissible delta variant, along with transfer patients from all over the state, has their system strained of resources and space past what they thought were limits six months ago.
The “younger and sicker” wave of COVID has the average ICU patient count at Memorial Hospital lingering around 16 or 17, said ICU manager Whitney Sutton. During the pandemic’s peak in January, when the Sun Herald last visited, 16 ICU patients was a hospital record.
“Right now is way busier than it was six months ago, The patients are getting sicker faster, they’re sicker than they were six months ago, and even though we know so much and know how to take care of these patients, it is busier. We have way more patients than we did, and we’re not even at the peak,” said Lewis.
Memorial is currently managing 38 ICU beds and 45 critical care beds. During the last wave’s peak, they had only managed 26 ICU beds. The hospital’s critical care unit, emergency room and other units are also caring for the “sickest of the sick” ICU patients.
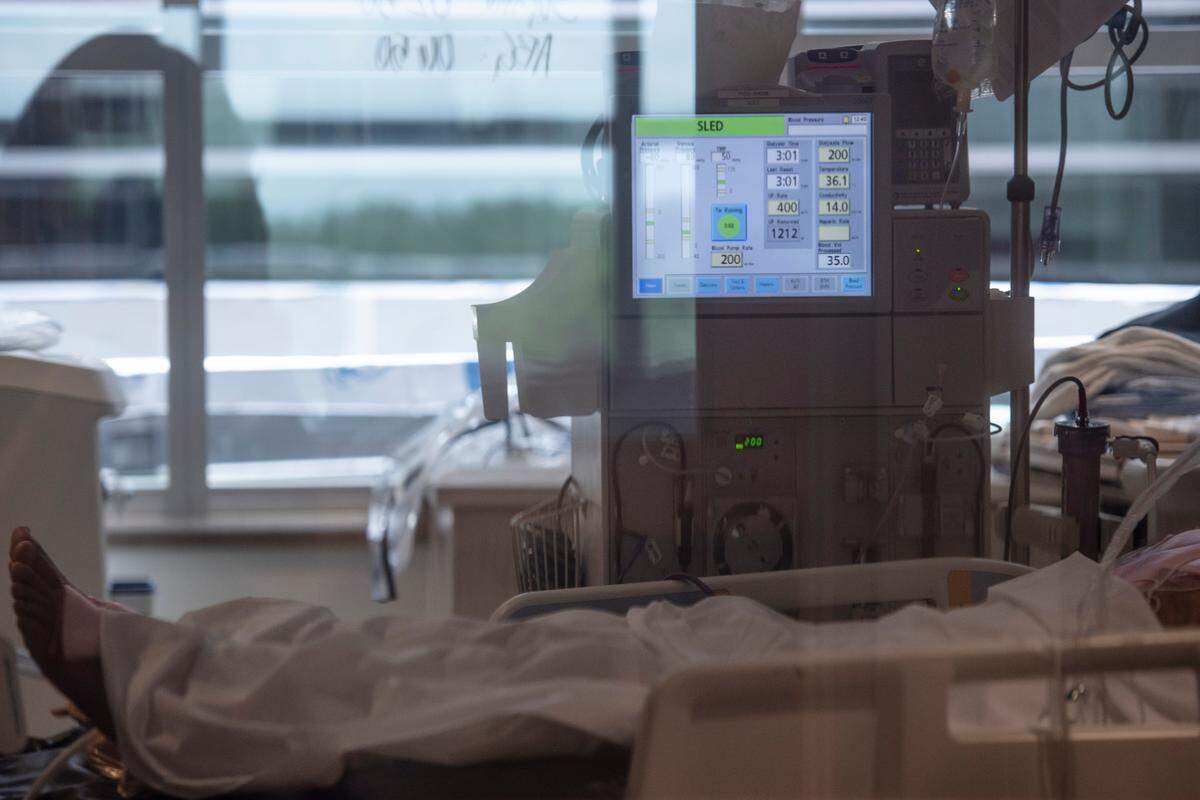
“We have so many patients. They’re in the ER. I have to go down and help the emergency room because they’re overwhelmed.”
The Rocky Balboa theme song, which echoes throughout the entire hospital whenever a COVID patient is discharged, played as Lewis put on her personal protective gear to prone a patient, or to flip them onto their belly in order to breathe easier. The song used to play a lot more, another ICU nurse said.
“Our patients stay with us. Last time it was months at a time, this time it doesn’t seem as long, just because they’re not living as long. We can’t keep them alive as long,” said Lewis.
‘Survival of the Fittest’ in swamped hospitals
When the Sun Herald spoke with Lewis six months ago, the pandemic was peaking across the country. Mississippi had some of the lowest COVID rates in the nation as vaccines were not yet authorized for the public.
Now, as the Coast grapples with the third highest mortality rate and one of the lowest vaccination rates in the nation, COVID cases are higher than they were in January, and the Mississippi has shot up to one of the highest cases per state.
The Coast’s vaccination rates trail the statewide average of 36% fully vaccinated individuals. Only 25% of Hancock County has received both of their doses. Harrison County is 31% fully vaccinated and Jackson County averages 30%.
“It’s survival of the fittest at this point,” said Lewis. “It truly is. If you chose not to get vaccinated, don’t complain about sitting in the emergency room for eight, nine, 12 hours at a time, trying to get seen.”
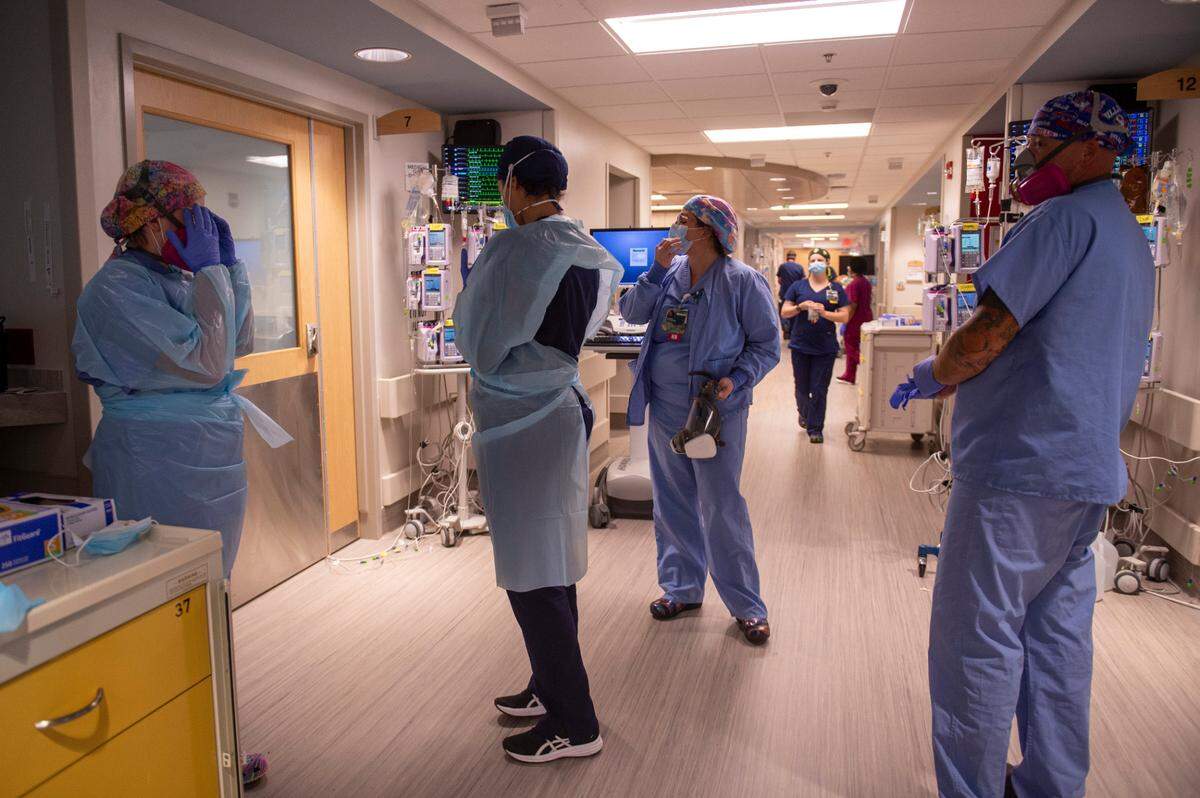
At Memorial, 98% of the hospital’s current positive patients are unvaccinated. In the ICU, 100% of the patients are unvaccinated, Sutton said.
Most of those patients are unable to communicate with the ICU nurses because of their conditions, but many have “begged” for the vaccine at the very end, said Lewis.
“They completely can’t talk to me because they’re on full life support with a breathing tube down. If they can talk to me, they’re so short of breath that they’re just begging. I’ve had patients beg me to take the vaccine. But it’s too late,” she said.
At that point, they’re so short of breath and they’re so miserable and they cannot catch their breath and they’re like, “Can you give me the vaccination?”
“Well it’s too late, you’re too sick.”

The age of patients has also proved shocking to the ICU nurses — the younger, less vaccinated age group has been a mainstay at the hospital. Memorial last week saw a 24-year-old patient in the ICU.
“We have kids in this ICU — I know a 24-year-old isn’t necessarily considered a kid… that’s someone’s baby that we’ve had in this ICU. And he was one of the people that we were able to make it out. But he is a minority in this situation. There are not many that make it out of the ICU setting when they have this,” said Sutton.
“Ages have ranged from very low 20s to 60s. We haven’t seen a lot of our elderly population because they got vaccinated.”
How Memorial has adjusted to statewide hospital mandates
The Coast’s elderly population is suffering in different ways, however.
In late July, the Mississippi State Department of Health put all state hospitals under mandates that delayed non-emergent medical procedures and initiated the state’s central transfer system. This system of care plan was extended as COVID continues to overwhelm the state.
Memorial has adjusted to these state mandates, Sutton said. Routine procedures for the elderly and other age groups, and even victims of strokes or heart surgeries, cannot be housed at Memorial because of the strain COVID has placed on the system.
“The strokes, craniotomies, the open-heart surgeries, all of these things that were routine procedures — we’re no longer able to house those patients because over half of our ICU population is COVID,” said Sutton.
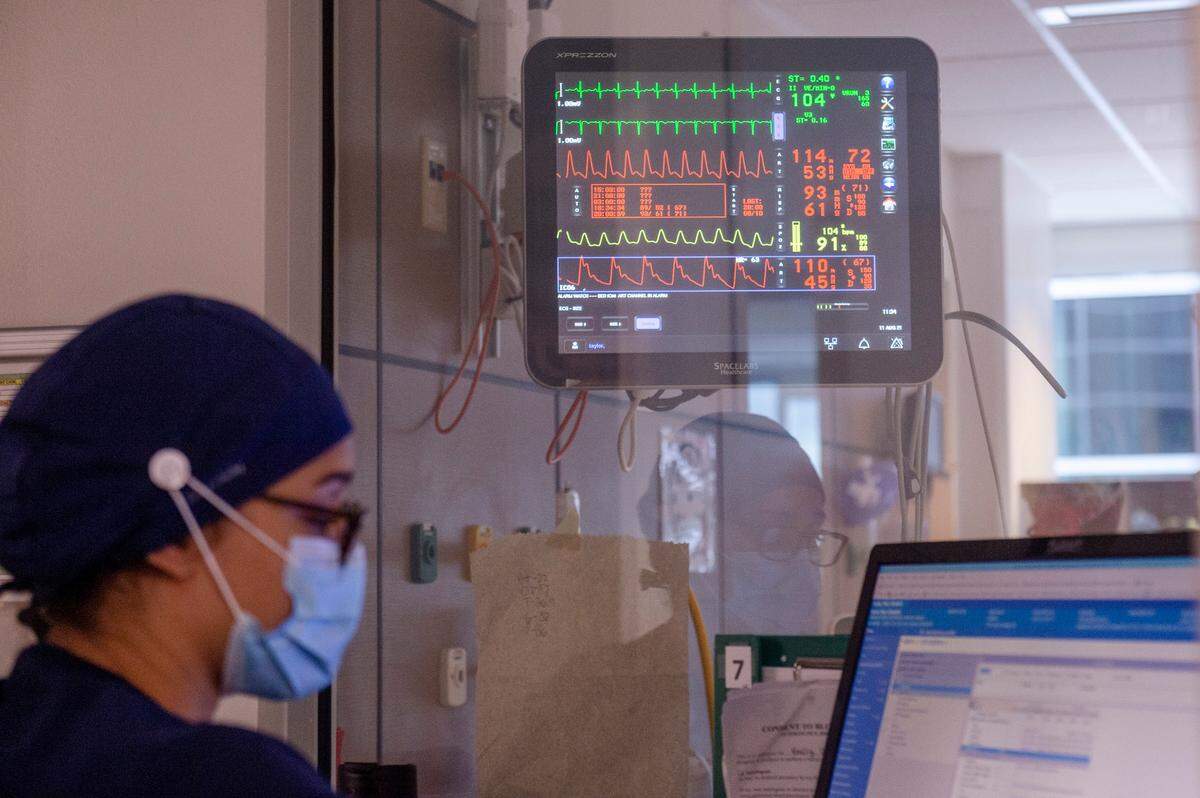
“They’re not being transferred, every hospital in the state and across the tri-state area are full with COVID patients… when those patients need those emergent procedures, we absolutely do them. If they come in the door and they need them done, we do them. Just the wait for them to actually get a bed is the issue.”
Memorial has turned away procedures that aren’t urgent or emergent, Sutton said.
A large reason that Memorial is so swamped is because of the Med-Com, or Mississippi’s central hospital transfer system, patients.
Memorial’s full ICU and overflow patients are largely because of that system, Sutton said. COVID or other types of patients come from all over the state — a few have also come from Bogalusa, Louisiana.
“Anybody that comes through these doors, we’re willing to take care of. It doesn’t matter if they’re from Gulfport Mississippi, it doesn’t matter if they’re from Bogalusa, Louisiana—wherever they come from, if they’re going to be taken care of, we absolutely do that.”
Staffing Shortages are also a real issue
Reeves did accurately describe the staffing shortages hospitals across the state are facing. Sutton said Memorial is also strapped for help.
A number of Memorial nurses have perused private contracts with travel nursing companies — a lucrative career option as the pandemic rages throughout all of the nation’s health systems.
“Some of the nurses are going traveling, there is financial gains to that. So they just want to explore the things, even if it’s in another place, still in the same exact thing. Just to kind of get another point of view,” said Sutton.
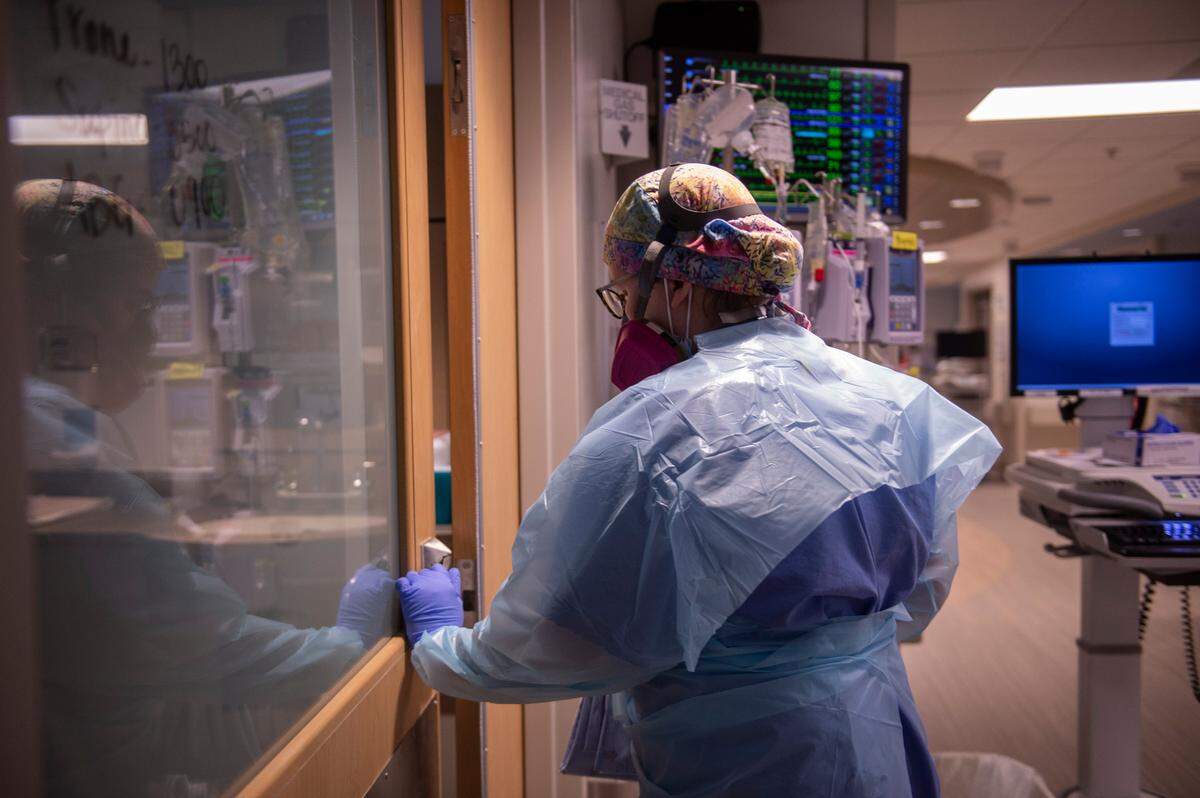
But the pandemic’s emotional and physical toll on nurses is also draining the hospital of their assistance. Sutton said “a lot” of nurses have left the ICU and have gone to other areas of nursing.
“We just have those nurses that at this point, have PTSD from the past year. Some have come to me and just said, ‘I can’t do this anymore.’ It’s not necessarily that they don’t want to be a nurse anymore, they just go into a different area of nursing,” she said. “They go to a clinic, they may be a school nurse. There’s so many different aspects of nursing that they can do.”
Patients come first in Memorial’s ICU unit, Lewis said, which has most nurses who are still in the ICU emotionally and physically drained amid staffing shortages.
“All I’ve had today is the coffee I brought in and Karen brought cheese-its. We don’t get real lunch. There’s no lunch break around here,” she said.
The staffing shortages have left nurses “very close” to a breaking point, Sutton said.
“There’s only so much that people can give before they say, I have to take care of myself. I have to be there for my family… they’re not taking care of themselves sometimes,” she said.

“There’s a lot of times, as manager, you turn into counselor. You turn into staff… just trying to make sure that we don’t leave our staff naked. We don’t just work 9-5, our business hours. We’re here until 2, 3 o’clock in the morning, we’re here working shifts.”
Lewis said the exhaustion has left her drained and frustrated, especially when she sees on social media the vaccine or COVID misinformation contrary to what she’s witnessing in the ICU.
“I don’t have the energy to argue about the vaccine,” she said.
“We’re all frustrated because of all of the misinformation. There is so much misinformation out there, about ‘why aren’t we using this drug and why aren’t we using that drug?’ And unfortunately, it’s not doctors in the trenches, it’s this one is speculating this and this one is speculating that.”
This article is supported by the Journalism and Public Information Fund, a fund of the Gulf Coast Community Foundation.
This story was originally published August 22, 2021 at 7:30 AM.
CORRECTION: At Memorial Hospital, 98% of the hospital’s current positive patients are unvaccinated. In the ICU, 100% of the patients are unvaccinated. An earlier version of this story contained a typo that made those percentage unclear.
