‘We’re right in the middle of it:’ Coast nurses describe the heartbreak of COVID in ICU
They were sharing a laugh, the registered nurse and her COVID patient.
He was picking on her about how many times she had to jab him before she found a vein. It took her only once the day before, he said.
One minute he was laughing, the next, he was dead. Tears well in her eyes at the memory. It was one of too many tragic moments on the COVID-19 intensive care unit at Gulfport’s Memorial Hospital, where nurses have acted as surrogate family, only one of the skills COVID-19 has taught them too well.
“I’ve held more hands, I’ve been to the morgue more in one year than I have in 15 years,” said registered nurse Miranda Lewis. “Yep. It’s real. It sucks.”
With so many cases, COVID-19 in Mississippi has pressed hospitals to their limits and beyond. At Memorial, a nurse and a critical care director told the Sun Herald, the staff has adapted in many ways demanded by this novel virus. Health care workers lean on one another because nobody else understands what they face.
Memorial has added beds for critical and less seriously ill COVID-19 patients, and employed incentives to bring on staff amid a nationwide shortage of nurses and respiratory therapists. Even with the added beds, a steady stream of COVID patients means cancer, heart and other surgeries must at times be postponed for lack of ICU space.
Emergency-room staff must weigh the competing needs of COVID patients with those arriving because of other illnesses, including stroke, trauma and heart attacks. COVID patients may wait hours — or days — in the emergency room for a hospital bed and patients are at times stationed on stretchers in the hallways.
The Memorial staff, in the view of Director of Critical Care Holly Rodriguez, is managing what, in retrospect, would have seemed impossible.
“We can go from having one or two patients needing beds to 20 patients needing beds in a matter of hours,” Rodriguez said. “Patients come to the emergency room. We try to get them well and let them go home, but when they’re too sick, obviously, they need to be admitted.
“There are many, many days when we are holding patients in the emergency room.”
“ . . . We get to the point that we put patients anywhere they can be accommodated. That includes in the hallways sometimes.”
More space created as COVID patients fill ICU
Memorial has been dealing with heavy caseloads off and on since March, when the pandemic began in Mississippi. An increase in hospitalizations always follows a rise in cases.
It’s all avoidable, as State Health Officer Dr. Thomas Dobbs reminds Mississippians on a regular basis. Still, cases in most of Mississippi remain extremely high and were especially so after the holidays.
In this environment, public health experts caution, everyone should wear a mask outside their homes, social distance outdoors and avoid indoor gatherings.
The biggest pet peeve for Lewis is hearing people say COVID is not real.
“It’s very frustrating because we are right in the middle of it,” she said. “You see the (case) numbers every day. I don’t pay any attention to it because the numbers are right here.”
Lewis is speaking in a hospital room with an empty bed, part of a unit that in pre-pandemic days housed orthopedic and neurology patients. Now, the unit is dedicated to non-COVID ICU patients because COVID patients fill what was once a 12- to 15-bed ICU.
In all, Memorial has added 24 non-ICU beds to treat COVID patients and increased total ICU beds from 26 to 38.
Last week, Memorial was almost at its ICU bed capacity, reaching a high of 36 patients. Almost half suffered from COVID.
Memorial also is part of a mandated statewide rotation of hospitals that accept critical COVID patients from areas where no ICU beds are available.
“We get those whether we have to hold them in the emergency department or we can place them in the ICU,” Rodriguez said. “We’ve felt at capacity for some time now, but last week was the first time we hit 36 patients.”
Like other hospitals, Memorial is dealing with a shortage of respiratory therapists and nurses.
“We’ve done all kinds of creative things to make this work — incentives, sign-on bonusues,” Rodriguez said. “We also provide a lot of support for our staff. We truly have the best staff anywhere, I believe. That teamwork and camaraderie is one of the benefits that they bring to each other, really.”
The hospital also is offering competitive wages to bring in traveling nurses, she said.
Ventilators a last option for saving patients
COVID-19 has challenged health care workers and support staff, even housekeepers, in new ways.
Lewis has been forced to shift her mindset out of emergency mode. There’s no more rushing into a patient’s room.
She has to save herself first by suiting up: medical gown over scrubs, gloves, mask or respirator, face shield.
And nurses must take everything they will need into a patient’s room at one time, because once they step out, they have to shed all that gear and repeat the process to re-enter. That goes for the housekeepers, too.
There is no time to waste.
“You’re pulled in 17 different directions,” Lewis said, “but you’re trying to do what’s best for every patient.”
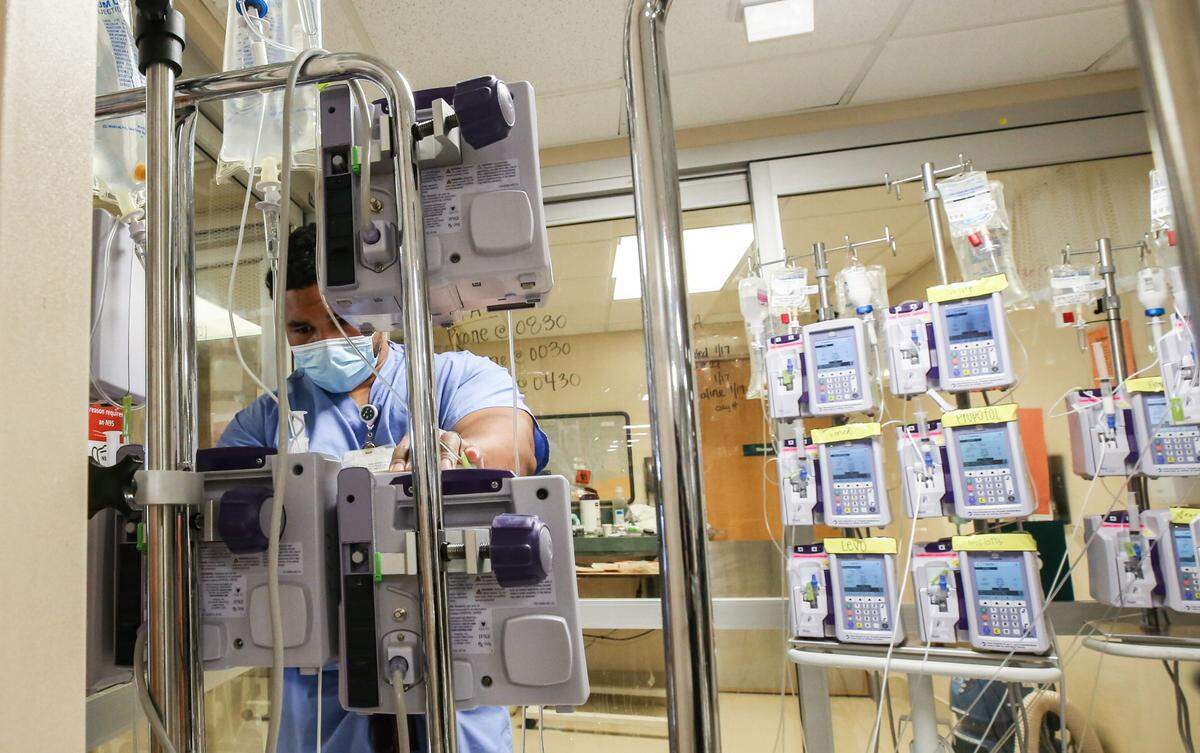
Caring for COVID patients is intense. One COVID patient might have 10 to 12 intravenous lines. The IV poles became so bothersome, nurses have learned to park them outside the rooms so they won’t bump into them.
Patients are turned onto their stomachs to help them breathe better, called “proning.” Turning someone over when they are hooked to mulitple IV lines and a ventilator can be tricky. It used to take six nurses 45 minutes, Lewis said. Now, three nurses can prone a patient in 10 minutes.
Lewis has treated COVID patients who have spent months in ICU. She knows the patients who must be put on ventilators have a lower chance of surviving, but COVID can ravage the lungs to the point that mechanical ventilation is the only option.

A study published in August by Clinical Infectious Diseases found the mortality rate for ventilated patients was 70.5%. Most of the 11,721 patients studied across the United States were men over 60 years old, and most were treated without ventilators.
Lewis said patients were put on ventilators sooner when the pandemic began, but the thinking changed as more patients were treated. The ICU team — including, intensivists (doctors who specialize in ICU care) and acute care nurse practitioners — tries to keep patients on ventilation that provides oxygen through a mask unless the patient can no longer draw breath to talk.
A mechanical ventilator forces air and oxygen into a patient’s lungs through a tube inserted in the windpipe. When a patient has to be ventilated, Lewis said, “We call that taking over.”
Patients on ventilators must be heavily sedated, with up to six medications, so their hyper-alert bodies can rest. They lay unconscious and immobile in Memorial’s COVID ICU unit.
Lewis spends 12-hour shifts in ICU with her patients and co-workers. She used to work three shifts a week but now works four to five.
Young people die of COVID, too
While most young people survive the virus, some don’t. The Memorial ICU staff recently lost a 33-year-old to COVID.
“Those are tough cases,” Rodriguez said. “They’re all tough cases.”
The staff also lost one of its own, 63-year-old Elaine McRae, whose children said she previously was healthy and never even caught colds. She was also extremely cautious, following all public health and hospital rules for avoiding COVID.
McRae, tended by the co-workers on the COVID unit where she had agreed to work, wound up on a ventilator in ICU. She had recovered somewhat, but died in November after 72 days in the hospital. The disease had destroyed her lungs, her children told the Sun Herald.
“We’ve seen so many people say goodbye to their moms, to their dads, to their aunts to their uncles, to their sisters, brothers. It’s very — ” Rodriguez searches for the word “ — very sorrowful.”
Statewide, Mississippi has lost only one person 17 or younger, and only one 4 or younger. But deaths climb in higher age groups. Deaths by age listed below are Mississippi State Department of Health statistics updated Jan. 27:
- 15 deaths — 18-24 years old
- 108 deaths — 25-39 years old
- 210 deaths — 40-49
- 1,027 deaths — 50-64
- 4,580 deaths — 65+
‘Wear your mask,’ critical care director cautions
What the Memorial staff hoped would be a sprint has turned into a marathon. But they are still standing and committed to caring for their patients.
Vaccines for COVID-19, Rodriguez said, have been “a gift.” For the Memorial staff, they came, appropriately, just before Christmas.
Nurses, physicians, all those touching COVID-19 patients, were vaccinated first.
“None of the staff resisted,” Rodriguez said. “They wanted that vaccine. They feel safer and they are safer.”
“ . . . The vaccinations have definitely given us hope. It’s been like that little beam of light that maybe, down the road, we’ll get through this and see the other side of it.”
Rodriguez wants people to know the coronavirus is not the flu but “so much more than that.
“This is not an illness that you want to see anyone that you love have.”
As the interviews at Memorial ended, Rodriguez was asked if she wanted to say anything else. She had this advice:
“Wear your mask.
“Get your immunization. Wear your mask. We wear these masks every day all day and we understand that sometimes it’s uncomfortable, but I assure you that it is nothing like you’ll experience if you’re here or you have a family member here. It’s not something that you want to go through.”
This story was originally published January 29, 2021 at 8:51 AM.
